We use cookies to improve your experience. By accepting you agree to our cookie policy


When you hear the term 'pacing' most people don’t know or understand what it means. People think that they don’t need to pace themselves to help with their CRPS or persistent pain, but in fact pacing is very important to help you do things better despite your pain. It is just one small part of helping you to self manage your CRPS or persistent pain.

Pacing can help you to take control of your condition and enable you to become an expert in managing your illness. What we mean when we say to pace yourself, is to not just put all your housework, jobs and activities in one part of the day, but arrange them throughout the whole day.
Many people living with persistent pain or CRPS or any other chronic illness will push themselves on those 'good days' so you try and catch up with everything that you may have not been doing. You feel that you have to get all your jobs and work load done before your pain becomes too much for you to handle and too much so you have to stop doing your jobs. However, one highly productive day could result in then next day or two, or even more, laying in bed or on the the sofa.
The challenge is how to get the jobs done productively without making yourself so tired or in pain that you can't do anything. This is where pacing can help. For example, instead of trying to all the housework in one hour of the day, try to do it in stages and spread the work over the whole day or even two days. This can allow for you to take frequent rests and move your body to avoid strain and reduce the chances of making the pain worse.
Activity doesn't necessarily mean physical activities, but also mental and emotional activities. Remember that pacing is a tool that you can use so that you don't react to pain but instead pre-plan your day to incorporate pacing.

Pacing for Complex Regional Pain Syndrome or chronic or persistent pain is a skill that can help you to carry out your jobs, work or activities without causing you extra and unwanted pain. It is a middle-ground between over-exerting yourself and doing nothing. Pacing means learning to break down your activities and jobs into small, manageable pieces without pushing yourself to the point where it causes a flare up of pain and other CRPS symptoms.
By learning to pace yourself, it will change the way you complete an activity or jobs so eventually you can increase your strength and your overall function, which is good for self-management of your condition.
When people over-do activities and end up with increased pain or flare up of your symptoms, it can result in pain patients stopping all activity or becoming highly inactive, through concern that it will just cause prolonged pain. This is not a good outcome. But, if you learn to pace yourself and split up your activities or work load and give yourself more rest periods, it will help you with managing your own condition.
Learning your own pain self-management strategies is crucial to the treatment of CRPS and chronic pain. It will eventually improve self-efficacy, enhance your quality of life and hopefully reduce your level of suffering (Jamieson-Lega, K. (2013).
The Jamieson-Lega, K. et al (2013) research study on pacing concluded that the definition of pacing for chronic pain is: "Pacing is an active self-management strategy whereby individuals learn to balance time spent on activity and rest for the purpose of achieving increased function and participation in meaningful activities."
The idea of pacing is to try and break the pattern of having less good days and more bad days as a result of pushing your body too much on those good days. You should be able to pace your way through any form of activity, whether it is shopping, hanging out the washing, hoovering or dusting the house or enjoying your favourite hobby, for example.
When you start pacing your activities and the jobs you have to do, you will find it hard, but eventually you should begin to be able to do them for longer and longer each time. Set yourself small goals and then increase them each day, but remember that you can say 'no' and ask for help. Also, remember to give yourself praise when you do attain your goals, no matter how large or small they may be.
Living with CRPS or a chronic pain condition means that whilst on some days you can feel less pain, there will be other times where your pain is worse or you're in a flare up of your symptoms. When chronic illness reduces your activity levels, it is very easy to try to make up for lost time on better days. Yet, cramming in too much activity on a day when you are feeling better often leads to a setback in your symptoms. It becomes a vicious circle or a Catch-22 situation. This is sometimes called 'boom and bust' or 'activity cycling'. (Pacing for people with M.E. booklet 2016)
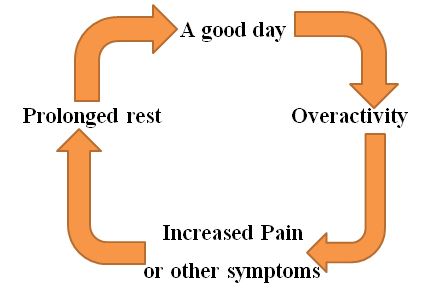
Pacing gives you awareness of your own limitations, which enables you to positively plan the way that you use your energy, maximising what you can do with it. Over time, when your condition stabilises, you can very gradually increase your activities to work towards recovery.
NICE defined pacing as: "…energy management, with the aim of maximising cognitive and physical activity, while avoiding setbacks/relapses due to overexertion…The keys to pacing are knowing when to stop and rest by listening to and understanding one's own body, taking a flexible approach and staying within one's limits; different people use different techniques to do this."
Most people may think pacing activity is just common sense, but managing activity with regard to CRPS and persistent pain is contradictory to the way you have lived prior to becoming unwell. You are generally taught to push through the pain when times get hard, to not stop and keep going. However, this sort of attitude does not work with CRPS or chronic pain. You need to learn to rest frequently to allow the body to recover energy.
If you push past your limit or 'Activity Baseline', your body sends out inflammatory responses. It is these inflammatory responses that cause you extra pain or indeed a pain flare up, causing agony over and above normal pain levels for a few hours up to a few days.
In the study by Neilson, W.R. et al (2001), they defined pacing to include going slower, taking breaks, maintaining a steady pace and breaking tasks into manageable pieces. Although the concept of pacing often includes the notion of increased activity tolerance, they viewed this as a consequence of pacing rather than as part of the construct itself.
The first important point to learn is what your personal maximum limit is for what you can do in any given day. Start by writing a daily diary of your activities, noting down the activity and the time it takes.
Self-management of your CRPS or chronic pain includes taking control of the balance of activity and rest, and learning how to communicate to other people about the balance that usually works best for you. This balancing out of activity and rest is sometimes called "energy management", "activity management" or "pacing".
Pacing is all about balancing your activity and rest to bring about more stability in your symptoms and, more importantly, what you can manage every day. It also offers you an opportunity to control the consequences of your CRPS or chronic pain. Whilst it does take self-control and patience, the stability it brings will help you to take decisions about building up activity (Action for M.E.2016).

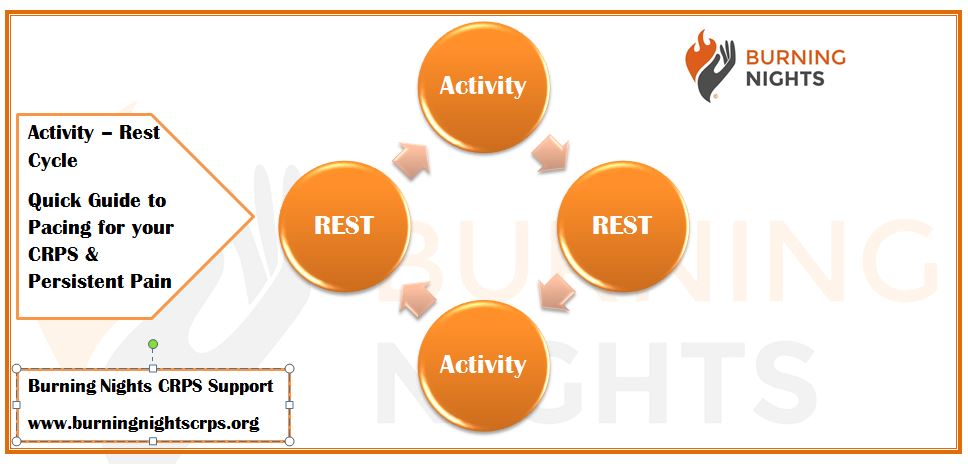
McCracken, L.M. & Samuel, V (2006) recommend that a formal approach to pacing would require training patients in certain steady rates of activity, perhaps without extreme fluctuations. 'Pacing' is seen as a poorly understood concept for which there are no available measures (Nielson, W.R. et al. 2001).
Check out the painHEALTH video on pacing and goal setting below:
You can also take a look at the Pacing Activity form created by VA Health Care.
By learning and understanding pacing for your CRPS or persistent pain, it could help you to be able to self-manage your condition. Our quick guide to pacing for your CRPS and persistent pain gives you that understanding to help you manage your condition and flare ups. You will improve with practice so remember to be patient as pacing takes time. Eventually, you will be able pace yourself without thinking and you’ll begin to wonder why you never learnt pacing for your CRPS or persistent pain before now.
*Burning Nights CRPS Support is a registered charity. We are not doctors or specialists and therefore cannot make any diagnosis, provide treatment, etc. You must speak to your doctor or healthcare professional before trying anything new or different to your usual pain management regime. This help is not meant to replace your current treatment regime or medication. If in doubt please contact your doctor or pain specialist first.*
*Burning Nights CRPS Support does not endorse any particular website, company or healthcare professional.*
Last Updated: 16/05/2020
We use cookies to improve your experience. By accepting you agree to our cookie policy
 £
£
